When Rachel Pope started studying the menopause transition a decade ago, she hadn’t lived it herself. So, she asked her three older sisters who they would turn to for help if they experienced the sleep problems, thinning hair, low libido and hot flushes that many women experience as their levels of reproductive hormone dwindle in midlife. “They said they would see a GP for some issues, a gynaecologist or dermatologist for others,” says Pope, a gynaecologist at Case Western Reserve University in Cleveland, Ohio. “I realized they were not connecting that all of these symptoms are coming from one collective situation, which is perimenopause.”
Perimenopause — the hormonally turbulent years leading up to a woman’s final menstrual period at around the age of 50 — is a tricky phenomenon to study. Retrospectively, menopause is easy to identify as 12 consecutive months without menstrual bleeding, but it’s harder to pin down while it’s happening. There is no clear biomarker or diagnostic test for perimenopause, and symptoms are highly individual. “We’re not good at treating perimenopause because we don’t completely understand it,” says Susan Davis, an endocrinologist at Monash University in Melbourne, Australia, who has studied menopause for decades.
This scientific uncertainty has consequences. Perimenopause is when debilitating symptoms such as hot flushes and ‘brain fog’ can be the most severe. But because most menopause research has focused on the years after periods stop, clinicians have little trial-based guidance for treating women whose hormone levels are still fluctuating. (This article uses ‘women’ to refer to individuals who go through the menopause transition.) The result is a landscape in which medical practice, public messaging and women’s expectations are all evolving faster than the research evidence is.

Gynaecologist Rachel Pope says that hormone therapy helps to relieve some of her patients’ symptoms, but that long-term effects are understudied.Credit: Kim Ponsky Photography
Treatment of perimenopause, for example, tends to focus on stabilizing hormone levels using either menopausal hormone therapy (MHT) or hormonal contraceptives to supplement the body’s drop-off in oestrogen and progesterone. But these approaches are mostly informed by postmenopausal studies, and have not been optimized for perimenopause, when people might respond differently. Indeed, says Davis, in some cases “giving more oestrogen can make things worse”, because women who are perimenopausal still produce variable amounts of hormones; adding more can cause them to “bleed all over the place”.
The lack of clear research around perimenopause has left a knowledge gap that some providers have filled with treatments that fall outside established clinical guidelines. Unproven hormonal treatments, such as pellets implanted under the skin, are marketed as quick fixes, and their risks are often downplayed. Testosterone, another hormone that declines as women age, is used by some women during perimenopause and menopause to alleviate symptoms such as low libido, brain fog or low energy. However, few studies have evaluated the long-term safety of testosterone to treat menopause symptoms, and physician guidelines advise against using it as a first-line treatment. Meanwhile, the long-term effects of starting MHT in perimenopause remain understudied. “I can tell you these treatments are helping my patients relieve their symptoms,” says Pope. “But I can’t tell you from our current data what that means several decades from now.”
Out of the shadows
Hormone therapy (see ‘From high doses to more precise relief’) has travelled a long road since 2002, when part of the Women’s Health Initiative (WHI), a large US randomized trial to test it, was stopped early. In a dramatic press conference, the researchers halted research, reporting that participants receiving combined therapy of oestrogen and a progesterone-like hormone had increased relative risks that ranged from 26% to 41% for the conditions breast cancer, heart disease and stroke compared with those given a placebo1. Millions of women immediately stopped treatment and physicians’ prescription rates plummeted, leaving women to navigate their symptoms almost completely unaided. But the alarming-sounding relative-risk numbers were widely misinterpreted: the increased absolute risks for any individual woman taking the therapy were small.
Two decades on, research has begun to correct the record. Reanalyses2 of the WHI data showed that the risks were even smaller than initially thought, and were linked mainly to older women receiving outdated hormone formulations. Last November, on the basis of these analyses, and after a decade-long campaign by menopause physicians and researchers, the US Food and Drug Administration (FDA) announced that it would remove its strongest ‘black box’ warnings from hormone-therapy products — these had scared many women off taking MHT. Major medical societies now agree that, for women experiencing symptoms around the typical age of menopause, hormone therapy’s benefits outweigh its risks.
But research gaps remain about MHT’s long-term health benefits and risks, especially for people who start it in perimenopause (see ‘Some of the benefits, risks and unknowns of hormone therapy’). And some researchers now worry that the pendulum is swinging too far the other way. Some social-media influencers are pushing oestrogen as a fountain of youth, and framing its depletion as a major culprit in ageing and ill health. And influencers aren’t the only source of misinformation. The FDA’s announcement in November trumpeted that MHT reduces Alzheimer’s disease risk by 35% and cardiovascular disease risk by 50% — claims refuted by menopause scientists. Petra Stute, a gynaecological endocrinologist at the University of Bern in Switzerland, called the FDA’s numbers “not that accurate” during a European Menopause and Andropause Society meeting last November.
Pauline Maki, a neuroscientist at the University of Illinois Chicago, studies how ageing affects the brain. She called the claim of a 35% reduction in Alzheimer’s risk “misleading and inaccurate in light of what we now understand” in a social-media post that she made to counter the FDA’s data, and told Nature that the data seemed to be taken from a single 1996 study. In December 2025, a systematic review of ten studies surveying more than one million participants found no evidence that hormone treatments affect dementia risk3.
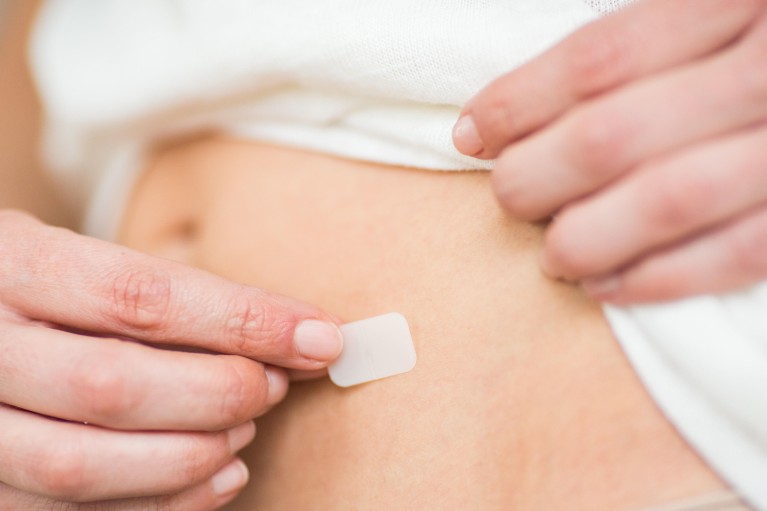
Transdermal hormone therapy is considered safer than taking hormones orally.Credit: Garo/Phanie/SPL
A spokesperson for the US Department of Health and Human Services, which oversees the FDA, responded to these criticisms in a statement: “Studies have provided evidence that for millions of women, starting HRT within ten years of the onset of menopause can have widespread benefits that outweigh risks.” The statement also referred to the Alzheimer’s study4, published in 1996, and the heart disease study5, published in 1991, cited in the original announcement.
Some long-term health benefits of MHT are undisputed. For example, decades of research have shown that starting oestrogen therapy around the time of menopause prevents the accelerated bone loss that begins in late perimenopause, thereby reducing fracture risk by 20–40%6.
The cardiovascular picture is more complex. Women’s cardiovascular disease risk increases after menopause — a phenomenon that has been attributed to oestrogen having a protective effect on heart health. Observational studies in the 1990s had suggested that MHT reduced the risk of heart disease7. But the WHI, designed to test this, initially showed no overall benefit and that there was in fact a short-term increase in cardiovascular events after hormonal therapy8. Reanalyses and later studies supported a 10-year window of opportunity, beginning at menopause or around age 50 for most women, for initiating MHT. During this window, MHT might confer modest cardiovascular advantages9. In particular, a 2016 study showed that women who started taking hormones in that time frame experienced a slowed progression of atherosclerosis, the constriction and hardening of blood vessels that can lead to heart attacks, strokes and blood clots10. But on balance, current evidence does not support the idea that MHT should be prescribed to reduce heart-disease risk, most menopause scientists say.
The bigger picture
Part of the reason for the continuing uncertainty around MHT for women and their physicians is that it is often difficult for researchers to work out which midlife changes are due to menopause, which are simply a part of ageing and which are the result of interactions between the two. “For example, does a particularly difficult transition lead to more or fewer health risks later in life?”, says Nanette Santoro, an endocrinologist at the University of Colorado Anschutz in Aurora.

Endocrinologist Susan Davis at the Alfred Hospital in Melbourne, Australia, says a lack of research around perimenopause means treating it can be challenging. Credit: Eva Mezel/Bayside Health Melbourne
Santoro is a lead investigator on the Study of Women’s Health Across the Nation (SWAN), which in the mid-1990s began following more than 3,000 women in the United States aged 42–54 to better understand the menopause transition and its consequences on women’s health. SWAN’s results show that some health challenges that were previously thought to be tied to menopause — such as weight gain, insulin resistance and cognitive changes — seem to track more strongly with chronological ageing than with menopausal stage. Although certain cardiovascular risk factors, notably cholesterol levels, rise around the time of menopause, SWAN shows that their contribution is modest compared with those of other risk factors, such as smoking and obesity. Meanwhile, midlife increases in depressive symptoms seem to be more strongly linked to mental-health history, stress and sleep disturbances than to changes in reproductive hormones alone.
The observational nature of SWAN means it cannot pin down causal links between the use of hormone therapy and health outcomes — and just 6% of its participants have used MHT. With SWAN’s cohort now in their 70s and 80s, the next data-collection cycle could prove pivotal for understanding which midlife factors affect health outcomes, Santoro says. “We will be able to measure actual disease instead of risk for disease, and that is a very valuable end point.” However, she and her colleagues have yet to secure funding for this final data cycle because the status of the project’s grant from the US National Institutes of Health, which must be renewed every five years, is still undecided.

Women often experience sleep disturbance during the menopause transition.Credit: SpeedKingz/Shutterstock
Another study, started in 2023, will include women even younger than those targeted by SWAN, and might, therefore, offer more insight into perimenopause specifically. The CLIMATÈRE study aims to follow more than 100,000 women in France aged 30 and older during a 20-year period to investigate the impact of menopause and its management on women’s physical, mental, metabolic and social health11. It will also collect data on the real-world use, benefits and risks of MHT.
Santoro thinks that what women really need is for researchers and physicians to gain a better understanding of the basic biology of perimenopause — “a sophisticated understanding of the root cause of symptoms and health risks,” she says. She would like to see explanations for why certain women experience worse symptoms, and ways to offer them relief that address the specific problems that they are facing. “Without that, we will forever be stuck with an oversimplified model that blames low oestrogen for everything,” she says.
Some scientists now think that it’s the hot flushes — not the drop in oestrogen — that lead to cognitive symptoms, such as brain fog, low moods and sleeplessness, during perimenopause and menopause. Although there is no clear-cut evidence for this, several studies suggest that there is a strong association. One of them is the Australian Women’s Midlife Years (AMY) study12, which surveyed 8,000 women aged 40–69 from October 2023 to March 2024. It found that women experiencing hot flushes had significantly worse brain fog, sleep disturbance, weight gain and low mood, compared with women at the same menopausal stage who did not. “If you don’t have the hot flushes and night sweats, you’re much less likely to have the other symptoms,” notes Davis, one of AMY’s research leaders. “It’s a cluster.”
Uncharted: Understanding women’s health across the body
Maki’s work supports this. Her research shows that the more frequently women experience hot flushes, the poorer their memory performance is, even when controlling for sleep13. In particular, night-time hot flushes were strongly linked to poor memory. In another study, Maki and her colleagues imaged the brains of 14 postmenopausal women with moderate-to-severe vasomotor symptoms (experiencing at least 35 hot flushes per week) while they performed memory tasks. The researchers found that, in people experiencing more-frequent hot flushes, their neural circuitry had to work harder to achieve the same cognitive performance as those who had fewer flushes14.

Endocrinologist Nanette Santoro leads a study of more than 3,000 women to better understand the menopause transition.
“If our theory is right, it really doesn’t matter if you treat the vasomotor symptoms with an oestrogen or an effective non-hormonal treatment. The point is that if you help women to sleep better, they’re going to function better,” says Maki.
This would be welcome news for the many women for whom MHT is not an option for medical reasons, or for those who do not wish to take it. Still, so many questions remain. “There’s a fundamental gap of information on the perimenopause,” Maki says. “We don’t yet understand how treating menopause symptoms, regardless of whether it’s hormonal or non-hormonal, benefits women or not.”
Pope admits it’s “incredibly frustrating” to be unable to answer some of the questions her patients ask. However, she’s glad that the tide is turning away from the hormone-treatment backlash of the early 2000s. “Women have been left in the dark regarding their options, and the risks [of MHT] have been blown way out of proportion,” she says. “Women should not be suffering with their symptoms. If there’s something they can take, we should be offering it.”



