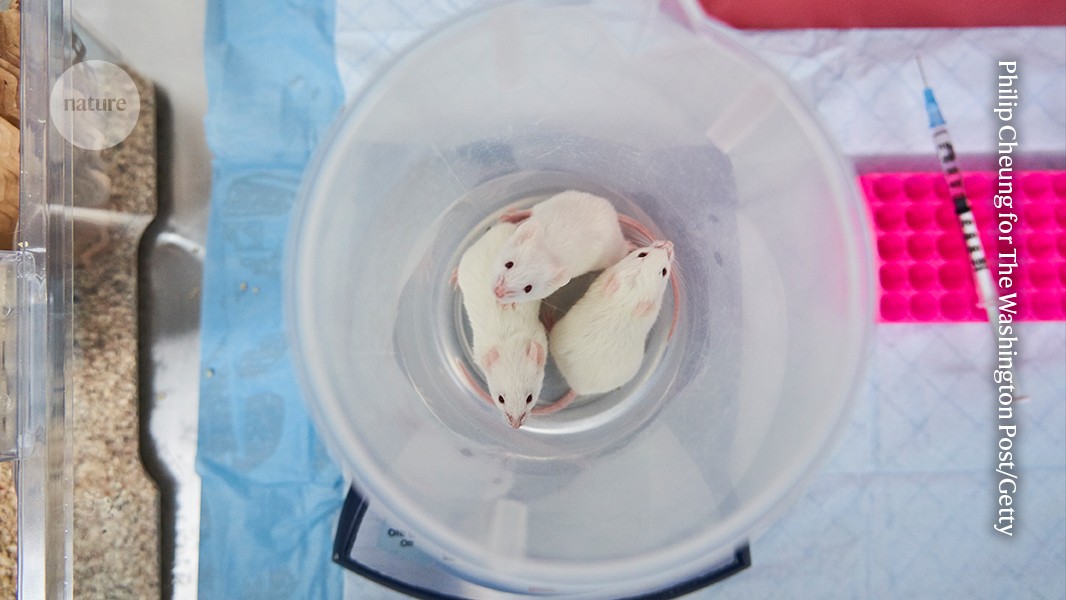
Last November, the UK government announced a bold plan to phase out animal testing in some areas of research. Animal tests for skin irritation are scheduled for elimination this year, and some studies on dogs should be slashed by 2030. The long-term vision is “a world where the use of animals in science is eliminated in all but exceptional circumstances”, the government policy reads.
Why simply ending animal testing isn’t the answer in biomedical research
Other nations are making similar moves. Last April, the US Food and Drug Administration (FDA) announced plans to make animal studies the “exception rather than the norm” in drug safety and toxicity testing in 3–5 years. The same month, the US National Institutes of Health (NIH) revealed an initiative to reduce the use of animals in research that it funds. This year, the European Commission plans to publish a road map to end animal testing in chemical safety assessments.
Ethical and animal-welfare concerns have long fuelled efforts to curb animal use in research — and now rapid advances in alternative scientific methods are accelerating the shift. These ‘new approach methodologies’ (NAMs) include devices known as organs-on-chips, 3D tissue cultures called organoids and computational models, such as artificial-intelligence systems. The number of biomedical publications using only NAMs grew from around 25,000 to 100,000 between 2006 and 2022, according to an analysis of studies on seven diseases by Animal Free Research UK, an organization that promotes the replacement of animal experiments1 (see ‘Alternatives on the up’). And China is investing heavily in this area: in 2024, it launched the Human Organ Physiopathology Emulation System, an infrastructure project dedicated to developing NAMs, backed with an investment of 2,640 million yuan (US$382 million).
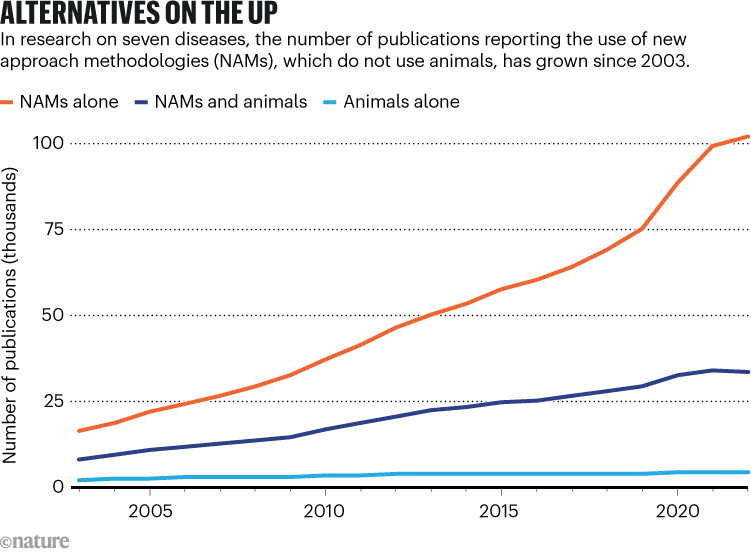
Source: Ref. 1
Proponents say that NAMs can be better than animals at mimicking human biology and predicting whether new drugs are safe and effective. Organs-on-chips and organoids are often created with human cells, and computational models can be designed using human data. The shift towards alternative models is “long overdue”, says Donald Ingber, a bioengineer at the Wyss Institute for Biologically Inspired Engineering in Boston, Massachusetts, and a co-founder of Emulate, a biotechnology company in Boston focused on organs-on-chips.
But NAMs are a long way from ousting all animal procedures in research, scientists say. Some biological systems are too complex and unpredictable to study without animals. And many of the alternative methods have yet to be validated — to show that they represent the system they are modelling accurately and reproducibly enough to satisfy drug and chemical regulators. “Not all of these [alternative] models are ready for prime time,” Ingber says.
On the decline
Efforts to replace, reduce and refine the use of animals in research (known as the 3Rs) have been ramping up for decades; in some places, use of animals is already falling. Data from the United Kingdom show that the number of scientific procedures on animals fell from 4.14 million in 2015 to 2.64 million in 2024 (see ‘Falling numbers’). The total number of animals used in research and testing in the European Union and Norway dropped by 5% between 2018 and 2022. (The number used in the United States is hard to pin down because the law does not require reporting on rats, mice and fish.)
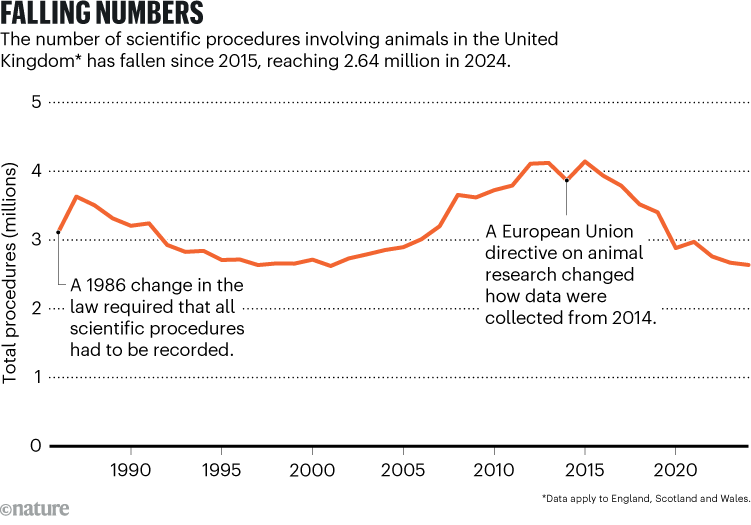
Source: Annual Statistics of Scientific Procedures on Living Animals, Great Britain 2024 (Home Office, 2025).
In the United Kingdom, around 76% of experimental animal procedures are for basic and applied research: understanding organisms, modelling disease and developing new therapies (see ‘What animals are used for’). Another 22% are part of regulatory procedures — mostly testing the toxicity and safety of new medicines and other chemicals before they can be used. Some 67% of all procedures involve mice or rats (see go.nature.com/3mzfkgw).
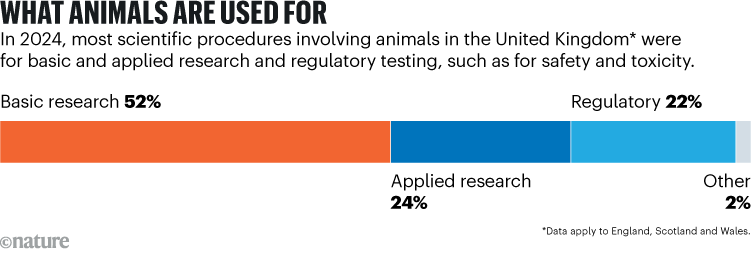
Source: Annual Statistics of Scientific Procedures on Living Animals, Great Britain 2024 (Home Office, 2025).
But these and other animals have limitations, especially when it comes to understanding and intervening in human diseases. Medicines that work in animal models during preclinical testing often prove ineffective in humans. This is one major reason that around 86% of investigational drugs fail in clinical trials2, and why many researchers are focused on developing alternatives.
Take sepsis, for instance, a severe reaction to infection. Researchers have developed more than 100 therapies for sepsis that looked promising in rodent models but that were ineffective in clinical trials3. That’s partly because of differences in human and rodent immune systems and the difficulty of mimicking a complex condition that varies from one person to the next in inbred mice that are genetically similar and raised in uniform conditions.
Increasingly, researchers see NAMs as a way to help. Joseph Wu, a cardiologist and researcher at Stanford University, California, and his team have been developing an approach that they dubbed “clinical trials in a dish”. This involves generating induced pluripotent stem cells (iPSCs) from a range of people with a medical condition, using these to grow cells or organoids and then testing whether potential drugs improve how the ‘diseased’ models function.
Alternatives to animal testing are the future — it’s time that journals, funders and scientists embrace them
In one 2020 study4, Wu and his team grew iPSCs and then endothelial cells — which line blood vessels — from members of a family carrying a mutated gene that can cause a common form of heart failure. Using these cells, the researchers were able to screen possible drugs and pinpoint one that helped to improve cardiovascular function in two members of the family with the mutation, and that might be used more widely. Integrating this method into a drug-development pipeline, says Wu, could help to reveal whether a drug works before animal testing, reduce the number of animals used and increase the success of clinical trials.
Studies suggest that some NAMs are as good as, or better than, animal tests. Emulate has developed an organ-on-a-chip system called Liver-Chip, a USB-stick-sized device in which human liver cells are grown in tiny fluid-filled channels and used to test whether potential drugs might cause liver damage. A 2022 study5 by the firm suggested that the chips could correctly identify compounds known to have caused liver injury with 87% accuracy, without falsely flagging harmless compounds as toxic. The chips also detected 12 of 15 liver-harming drugs that were previously, using animal models, deemed safe enough to proceed to clinical trials.
Animal research is not always king: researchers should explore the alternatives
In 2024, Liver-Chip was accepted in the FDA’s Innovative Science and Technology Approaches for New Drugs (ISTAND) pilot programme, which supports the advancement of tools for drug development. If approved, pharmaceutical firms could use the chip to test for toxicity in place of animal models and submit the data as part of a drug-approval application.
Such chips are highly specialized, however. Edward Kelly, a toxicologist at the University of Washington in Seattle, and his colleagues developed a kidney chip that can reproduce aspects of acute kidney injury in humans6 and that is being considered for the ISTAND programme. But the device includes only one of the kidney’s more than two dozen cell types, he says. “It’s a reductionist approach, which allows us to study those cells in greater detail. But understanding what happens in the whole human kidney still requires animal studies,” he says.
Organoid options
Another popular alternative to animal testing is organoids — 3D living systems that capture many of the features of real tissues or organs.
Over the past decade or so, researchers have created a wide array of organoids that can model human diseases, including cancers and genetic disorders such as cystic fibrosis — and used those to screen for possible drugs and test for toxicity. In a 2021 study7, researchers generated human liver organoids using iPSCs. They used these to create a toxicity screening tool that detected substances that curbed the organoids’ bile transport and mitochondrial function. The assay was highly accurate when tested on 238 marketed drugs.
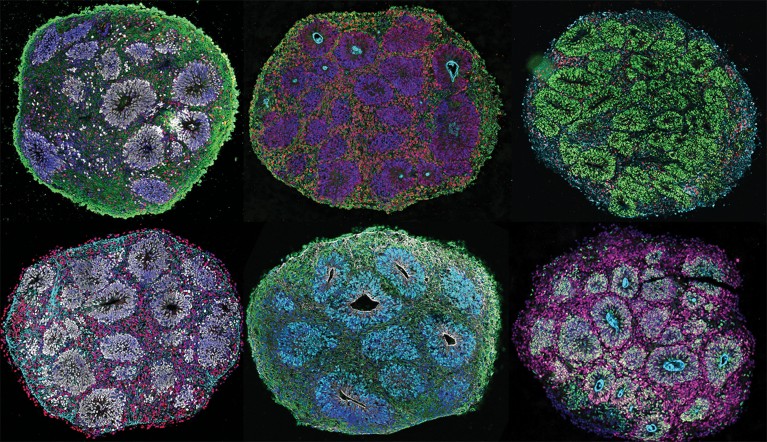
Human brain models and other organoids could reduce the use of animals in research.Credit: Noelia Antón-Bolaños, Irene Faravelli, Rahel Kastli/Arlotta Lab
And a third alternative is computational models, in which researchers test how a drug behaves in silico. In 2021, a team developed a tool for testing whether a compound causes skin sensitization — an allergic reaction in people. This is a standard part of safety testing for chemicals in industrial and household products and medicines, and conventionally requires animal tests. The team built a virtual test using data on around 430 chemicals from previous human, mouse and laboratory studies, and showed that it could accurately identify chemicals with a 1% chance of causing a skin reaction8. The tool was accepted as an approach for skin-allergy testing last year by the Organization for Economic Co-operation and Development, which sets internationally recognized guidelines for safety testing chemicals.
Researchers hope that AI can help too. Several regulatory agencies, including the FDA and the European Medicines Agency (EMA), are working on integrating AI tools into their chemical or drug safety-assessment pipelines.
Mini hearts, lungs and livers made in lab now grow their own blood vessels
In 2023, researchers at the FDA’s National Center for Toxicological Research in Jefferson, Arkansas, and their colleagues used clinical data on more than 8,000 rats treated with 138 compounds to build a generative AI model called AnimalGAN. In a simulated experiment involving 100,000 virtual rats, the team showed that the model could correctly rank the liver toxicity of three drugs with similar chemical structures9. This approach is now part of a broader programme at the agency to advance the use of AI tools in toxicology.
The pharmaceutical industry is increasingly investing in NAMs. Marianne Manchester, global head of pharmaceutical sciences at the multinational drug company Roche in Basel, Switzerland, says that the firm has a growing number of studies using NAMs to test drug candidates in areas such as oncology and immunology. In 2023, the company launched the Institute of Human Biology, which is developing human model systems, including organoids, to speed up drug development. Animal data are still mandatory for most new drug applications for marketing approval in the United States and Europe, but the company has waivers to use NAMs data for 12 submissions to regulatory authorities, including the FDA and EMA, Manchester says. “There is much more openness to considering these alternative approaches.”